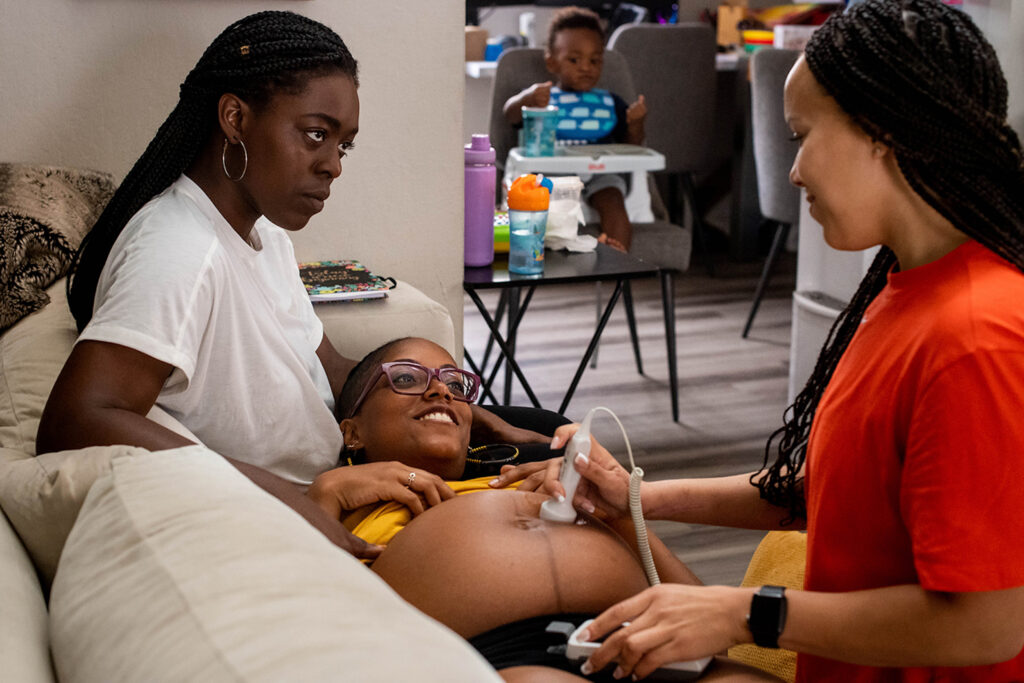
How Eugenics Shaped the U.S. Prenatal Care System
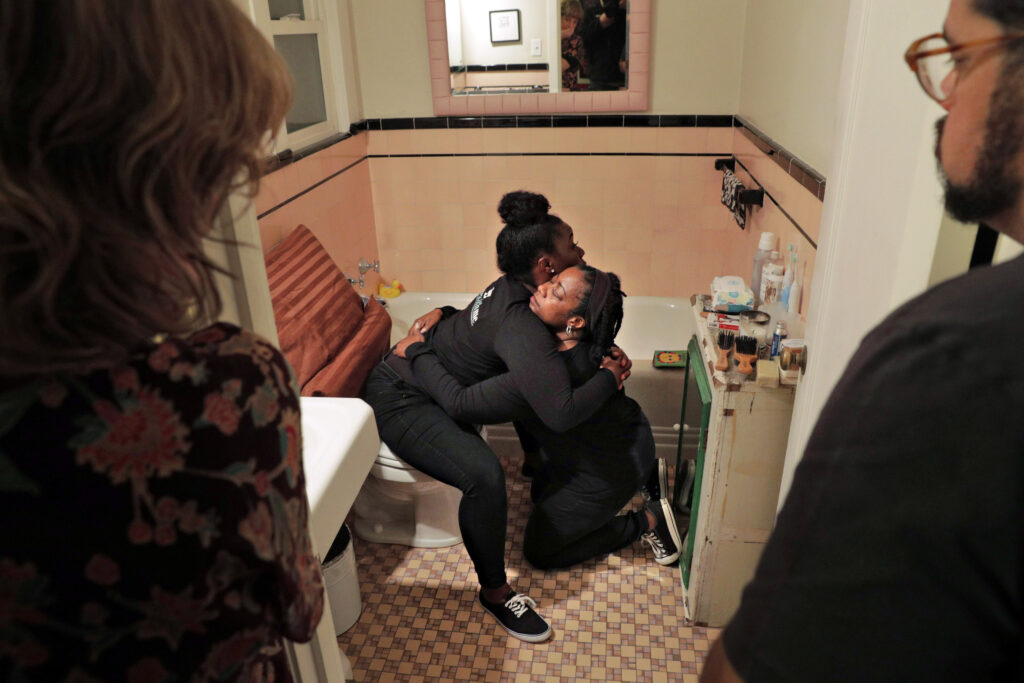
Ashley had a sense that something was wrong with her pregnancy during her second trimester. [1] [1] All names have been changed to protect people’s identities.
She was alone at her appointment when she requested an ultrasound. Her doctor refused to order it under the pretense that an ultrasound might harm the baby, even though medically necessary ultrasounds are generally performed without any evidence of injury to the fetus. Then one night, Ashley began to bleed profusely. She made an emergency visit to the hospital and was diagnosed with hypertension.
Ultimately, at 26 weeks, she had to have an emergency C-section because of placenta previa, a condition where the placenta partially or completely covers the cervix.
When she got pregnant for the second time, Ashley had a different OB/GYN whom she told about her past pregnancy complications. When she again received high blood pressure readings, the doctors assumed it was due to “lifestyle factors” such as having to take public transportation or working a job that involved standing. Neither of these were true.
Ashley again had to be rushed to the hospital to give birth early, this time with preeclampsia. The doctors spoke in ways she did not understand. Ashley was not unfamiliar with “medical talk,” as she called it; her grandmother and aunt were nurses. But Ashley’s medical professionals did not translate their jargon for her or ensure she knew what was happening.
In assessing both situations, Ashley, who was 19 years old when I (Davis) interviewed her, felt dismissed for being young and Black. Ashley knew she should have been monitored more closely. Yet the doctors in charge of her prenatal care showed little concern for her health history and current well-being.
Ashley is far from alone in feeling this way. For my (Davis’) book Reproductive Injustice, I interviewed many Black women who reported feeling harmed and neglected by the U.S. medical system. [2] [2] In this article, we primarily use “woman,” as all the people Davis interviewed identified as women. We also use “birthing people” to acknowledge that the experiences of pregnancy discussed here may be shared by trans men and nonbinary people.
Research across various fields confirms these racial disparities. For example, a recent New York Times article based on a new study reported, “In the United States, the richest mothers and their newborns are the most likely to survive the year after childbirth—except when the family is Black.” The study of 2 million first-time mothers in California found that despite access to some of the most comprehensive health care in the country, Black women were more than three times as likely as non-Hispanic White women to die from causes tied to pregnancy. Their infants also faced higher mortality rates, regardless of parental income.
To learn more about Davis’ work, check out this interview from our archives: “Broadening Demands for Reproductive Justice.”
This data builds on similar research that shows more than 4,000 Black babies die annually due to the racial gap—a disparity between White and Black infants that is greater than in 1850.
These findings support the groundbreaking work anthropologists Leith Mullings and Alaka Wali published two decades ago on health disparities among Black women. Mullings and Wali’s research in New York City’s Central Harlem neighborhood showed that the particular racism permeating Black women’s lives cuts across class and impacts their health outcomes.
But why do Black women face such disparities in their reproductive care? To start to answer that question, we need to understand the troubling history that led to the United States’ current prenatal care system.
THE EUGENIC ROOTS OF PRENATAL CARE
For centuries in the U.S., most women gave birth at home under the care of midwives.
This started to change in the mid-to-late 1800s as maternity wards in hospitals became more commonplace, and the fields of obstetrics and gynecology started becoming professionalized. Pregnancy and birth went from being under the care of midwives—often Black, Indigenous, and immigrant women—to being medically managed by White, male physicians.
Prominent White, male physicians and politicians helped put in place systems and policies to manage maternal health. While mainly intended to benefit White women, said systems and policies discredited or even criminalized “uncredentialed” midwifery. They especially targeted Black midwives. During and after enslavement, Black midwives played a fundamental role in women’s reproductive health, especially but not only in the South. Their skills, competence, and compassion were essential to community survival. However, White, male physicians and medical journal articles often painted Black midwives as dangerous and unclean.
Moreover, physicians increasingly relied on procedures that had to be done under medical supervision. This included administering narcotics and other drugs during and after labor, using forceps, and conducting surgical procedures such as episiotomies.
Digging a little deeper into what motivated the discrediting of Black midwives, we find that some of the architects of the current prenatal care system were eugenicists.
Fred Adair, who was born in 1877 and died in 1972, for example, was a prominent White obstetrician-gynecologist who helped pioneer the medicalization of birth in the U.S. While he recognized in the early 1930s that certain circumstances made midwives necessary, he viewed them as a temporary stopgap until physicians could have complete birthing authority, even in rural areas. He also actively supported eugenics and wanted to control women’s reproduction to “be able to prevent the birth of those who are defective and constitute a burden or menace to society.”
The basic philosophy of eugenics, according to science journalist Angela Saini, is the promise of a “bold new world filled only with beautiful, intelligent, productive people.” How is this achieved? By controlling reproduction and developing policies and practices that keep “undesirable” humans from living among “us” or reproducing. Eugenic policies can range, for instance, from sterilizing certain groups to promoting laws that support more “desirable” people’s survival.
Black midwifery’s near decimation is a loss that continues to reverberate throughout the current model of prenatal care.
Adair and his fellow eugenicists believed in eliminating or segregating people who they considered a “waste” to humanity. They believed Black people were racially inferior and that controlling human reproduction through medicalization was key to accomplishing their goals.
Adair helped orchestrate legislation that played a pivotal role in U.S.-based prenatal care: The Sheppard-Towner Act of 1921. Through the bill, each U.S. state received US$5,000. The goal, reliant upon education and increased access to nurses and doctors, was to help combat maternal and child health problems.
The federal legislation also regulated midwives; some states mandated midwives attend nursing school and work directly under the supervision of physicians. Many of these programs did not allow Black women to be certified, further delegitimizing the role of Black midwives.
By the 1930s, American midwifery had been reduced to a fraction of its original workforce. Today, according to a 2020 report by the American Midwifery Certification Board, less than 7 percent of midwives are Black. [3] [3] This number includes registered certified nurse midwives and certified midwives but does not account for certified professional midwives or lay midwives.
ADVOCATING FOR ALTERNATIVE CARE MODELS
Black midwifery’s near decimation is a loss that continues to reverberate throughout the United States’ current model of prenatal care. Given that Black people continue to be disproportionately harmed during pregnancy and birth, U.S. society needs to fully grapple with the consequences of this loss. Only then can we make room for more just and safe models of prenatal care.
Even as overall maternal mortality rates have decreased and other measures have improved since the early 1900s, racism and sexism heavily shape today’s medical care systems. While eugenics has been discredited over the past century, many of the maternal and prenatal care policies created by eugenicists such as Adair remain in place. These protocols include individualized medical supervision and monthly visits to a physician but often do not include access to other modes of supportive care.
How might Ashley’s pregnancies have turned out differently if she had access to a more holistic model of care—one that centered her emotional safety? What if she had been monitored by a midwife and supported by a doula, a person who provides nonmedical emotional care, instead of or in addition to a medical physician? What if she had been involved in group prenatal care that had offered social support and risk assessments?
Integrating midwives, doulas, and group prenatal care have repeatedly been shown to be very effective methods for improving birth outcomes and health equity, particularly for Black and Brown birthing people. Studies looking at midwifery globally have documented that access to affordable, community-based midwifery care can be lifesaving for parents and infants.
While many in the medical field tried to diminish midwifery, midwives still exist. In fact, Black midwives have been very intentional about providing services to members of the Black community.
For instance, in Illinois, where Ashley lived, a midwife from the Melanated Group Midwifery Care project or a doula from the Chicago Birthworks Collective would have likely paid more attention to her and her concerns. These kinds of group care and midwifery models center on empowering birthing people by democratizing active participation in care and fostering the development of peer and professional relationships. In other words, Ashley’s concerns would have been heard, and she would have received support.
As scholars and reproductive justice advocates, we want the public and policymakers to understand that these alternative care models already exist. Moreover, they have been shown to work better and keep Black birthing people safer and healthier than existing individualized prenatal care models.
One step we recommend is increasing government support for group prenatal care and midwifery, including establishing free-standing birth centers developed and staffed by midwives. [4] [4] There are five types of midwives in the U.S.: certified nurse-midwives, certified midwives, certified professional midwives, direct-entry midwives, and lay midwives. We advocate expanding support for all types of midwives. Passing the Black Maternal Health Momnibus Act, a series of legislation introduced by Rep. Lauren Underwood that is currently making its way through the U.S. Congress, would be a promising first step toward realizing these goals. We also support the National Health Law Program’s Doula Medicaid Project, which is fighting to expand Medicaid reimbursement for doulas in all 50 states.
These kinds of efforts are some steps in providing care that is more comprehensive and preventative for Black and Brown birthing people whose knowledge and needs the U.S. medical system has neglected for far too long.