What’s Behind Match Day’s Algorithm?
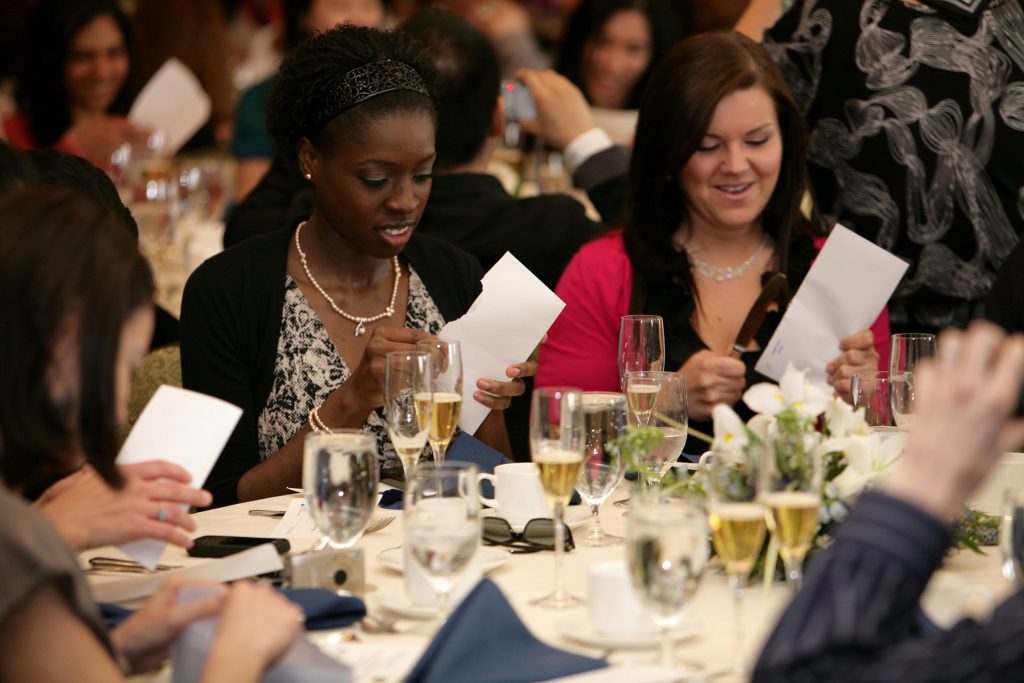
“Hmm, difficult. Very difficult. Plenty of courage, I see. Not a bad mind, either.
There’s talent, oh yes. And a thirst to prove yourself. But where to put you?”
—The Sorting Hat, Harry Potter and the Sorcerer’s Stone (film)
This week, students in their final year of medical school will gather across the United States in the Zoom equivalent of banquet halls, anxiously awaiting an envelope that will determine the next three to seven years of their lives. Held every year on the third Friday of March, Match Day is a rite of passage in the most classic anthropological sense. It is the day medical students find out where they will complete their residency training and transition from student-doctor to practicing physician.
The anxiously awaited envelopes (or, during the time of the pandemic, emails) not only tell students where in the country they will go but also what kind of doctor they’ll become. Will they be a surgeon in Chicago? An internist in Seattle?
This ritual is not unlike the one involving the Sorting Hat from the Harry Potter book and film series. The talking hat assigns arriving students to “Houses” at Hogwarts, a school for witches and wizards, by magically divining their true selves. Similarly, the Match Day envelope contains the name of the residency program that is the student’s most ideal match. This match is determined by a computerized mathematical equation, called the “matching algorithm,” but many students feel their results reveal something deeper than just an algorithmic output.
I first learned about the matching algorithm from my partner, who is now a first-year medical resident. This time last year, he was one of more than 40,000 medical students anxiously awaiting a match. I was anxious too. Though I was not the applicant, this algorithm had ramifications for my life as well. So, as we waited for Match Day to arrive, I channeled my nervous energy into anthropological curiosity. As an anthropology doctoral student who studies digital technologies in the U.S. medical system, I wanted to know: What makes a residency match “ideal”?
In other words, how does the matching algorithm answer, for tens of thousands of aspiring doctors, the Sorting Hat’s rather agonizing question: “But where to put you?”
Here’s how it works: After applying and interviewing at programs in their desired specialty (and in backup specialties as well), students rank each program according to what economists such as Alvin Roth—who won the 2012 Nobel Prize in economics for developing the matching algorithm—call “true preferences.” The matching algorithm then looks at the lists, placing each student into the highest-ranked program where the preference is mutual.
For economists, the matching algorithm represents a neat and tidy solution to a tricky labor market problem: What is the most efficient way to place newly graduated medical students into residency programs?
For students, the matching algorithm, colloquially called “the Match,” can mean something else. In the weeks leading up to my partner’s Match Day, friends, family, and other medical students frequently assured us that my partner would end up “where he was meant to be.”
These kinds of reassurances, which frame the Match as a technology of destiny, were not unique to our experience. Take this video of Stanford University’s Match Day event, titled “A Day of Destiny for Medical Students,” as an example. In the video, the clock counts down to the exact second when students around the country are allowed to open their envelopes. After panning around a banquet hall filled with people crying and hugging after opening their envelopes together, the camera cuts to sisters, both of whom matched into the same prestigious program. One says, “As fate would have it, we are both going to UCSF [University of California, San Francisco]. … It was meant to be to stay together.”
Where economists view the matching algorithm as an efficient and rational system, for students anxiously counting down the days, minutes, and even seconds until they open their envelopes, the Match symbolizes something both more mysterious and intimate: fate. This perception of algorithm-as-destiny is further cemented by the rules of the Match: If you renege on your assignment, you cannot reenter the market in the future.
Whether lauded as a hyper-efficient marketplace or revered as a technology of destiny (or both), the matching algorithm can start to seem more-than-human. It might even seem magical. Unlike the Sorting Hat, however, algorithms aren’t magic. As anthropologist Nick Seaver writes, “Press on any algorithmic decision, and you will find many human ones.” The residency matching algorithm is no exception.
It is easy to see how the decisions that students and program directors make as individuals influence their rankings. To create the ideal match, students are supposed to do the work of the Sorting Hat, each probing their “authentic” self to identify which program is the “best fit.” Program directors are supposed to do the same on behalf of their organizations. Yet upon closer inspection, the picture becomes more complicated. Preference lists are shaped by human decisions that extend far beyond the individual self.
Take, for example, the change that the National Resident Matching Program (NRMP), the organization that coordinates the Match, made to the matching algorithm in the 1980s. During the prior decade, participation in the Match among students had started to drop, which concerned the NRMP leadership.
Roth credited this decline in participation to demographic changes in medical schools: As more women entered the field, there were more medical school couples, and these couples often preferred to live in the same place. In a 1980 letter to the editors of The New England Journal of Medicine, one pair of medical school spouses called on the NRMP to recognize the “unnecessary agony” of their predicament, concluding that “human agency is preferable to the machine here.” Rather than participate in the Match—and risk ending up in different locations—couples started circumventing the program, reaching out to hospitals directly to negotiate jobs.
By acting outside of the Match to secure positions, couples threatened the stability of the matching algorithm. The system only works, after all, if everyone participates; students and programs must both believe the Match is the best way to get the ideal outcome. To restore faith, the NRMP added an option in 1984 for couples to submit preference lists together, guaranteeing they would end up in the same place.
Whether they participate in the Couples Match or not, students’ preference lists are shaped by their responsibilities and relationships to others, and by their social and economic circumstances.
Does a student have a child who has finally made friends at school or perhaps a parent in need of care? Do they have the financial resources to fly around the country for interviews? If they’re part of a same-sex couple, will they feel comfortable moving to a socially conservative area? Depicting the matching algorithm as the ultimate expression of an individual’s true preferences misses the complicated ways that people make decisions as members of communities.
At the same time, treating the matching algorithm like a technology of fate obscures how Match Day results—like the rest of a physician’s career—may be shaped by dominant cultural ideas about who makes “good” doctors, which often reflect stereotypes about race, ethnicity, class, age, and gender.
It is “vital to question which humans are prioritized in the process,” sociologist Ruha Benjamin writes.
On the residency interview trail, for instance, medical students report being asked questions about where they are from, what their spouse does for a living, and whether they plan to have children. Though the NRMP rules prohibit “discriminatory or coercive questions,” studies have found that, in practice, “potentially discriminatory topics are frequently discussed during both formal and informal interview events across all medical specialties.”
In a society that views some qualities as more “doctor-like” than others, even seemingly benign questions, like what an applicant enjoys doing in their free time, can influence whether a medical student is perceived by program directors to be a good fit. Tracing precisely how questions like these affect any one student’s performance in the Match can be difficult, especially when the ranking process is masked by the neutral and objective veneer of an algorithm.
Yet, as sociologist Ruha Benjamin writes about technology design, it is “vital to question which humans are prioritized in the process.” That means paying close attention to how social values and hierarchies influence the algorithm that determines what matches are supposedly meant to be.
Anthropology offers a set of tools for rethinking the residency matching algorithm: It reveals that the students and program directors participating in the Match are not theoretically rational actors but real humans embedded in the complexities of social life. Seen from that angle, the Match is not a perfectly orderly system or an agent of destiny but rather a complicated layering of human decisions hidden behind computer-generated ones.
In other words, algorithms alone do not decide what kind of doctor a student will become. People do.





























